In the 2018 United States Census, just shy of 290,000 of Minnesotans are age 65 or older. In 20 years that figure is projected to top 1.3 million. This population is at the greatest risk for sustaining a fracture of the hip, spine or wrist due to a fall and has the least physiological reserve for recovery.
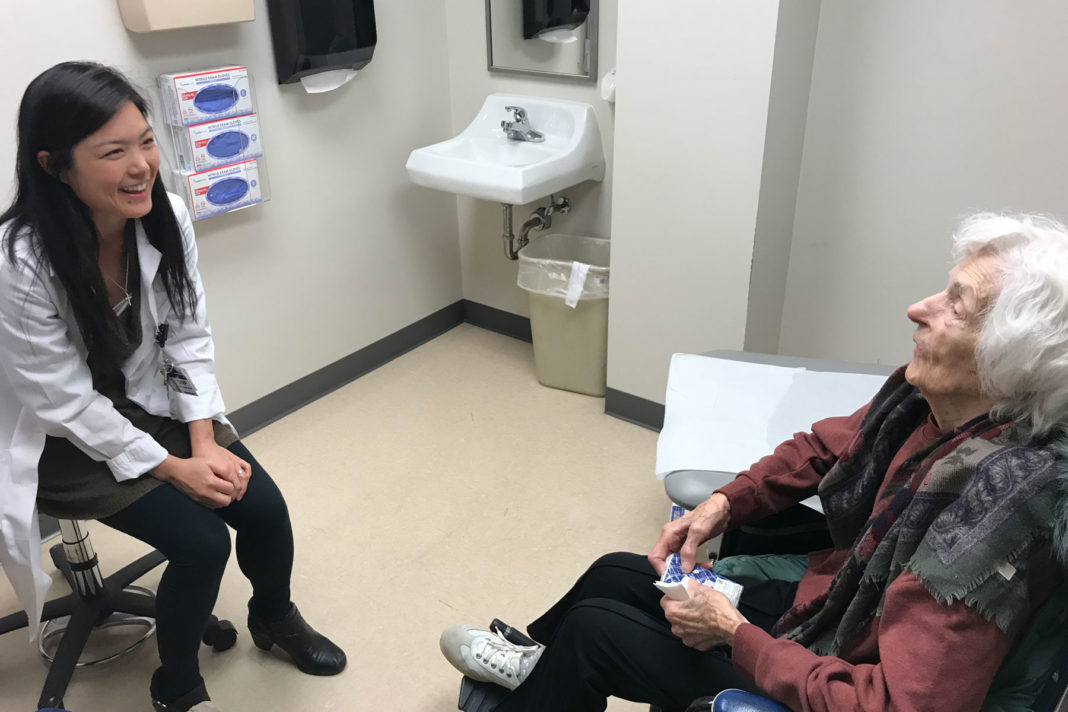
Medina resident Elizabeth Abell is directly involved in a new mobile orthopedic program through a collaboration of HealthPartners and the University of Minnesota, Regions and Methodist hospitals and Park Nicollet clinics aimed at caring for our older population who sustain fractures caused by falls. Abell coordinates the Mobile Outreach program for the western half of the Twin Cities, one of a three part Master’s Orthopedic Program developed by Dr. Julie Switzer. “Dr. Switzer’s specialties focus on care for the older orthopedic patient with musculoskeletal injuries, bone health and upper extremity orthopedic surgery including trauma and shoulder arthroplasty. Dr. Switzer is the latest surgeon to join Methodist as a traumatologist,” Abell says. “She had worked for many years at Regions (level 1 trauma hospital) prior to coming to Methodist. Her patients love her and a lot of them followed her to the west metro from the east.” Dr. Switzer is a board certified orthopedic surgeon, associate professor at the University of Minnesota Medical School, HealthPartners Medical Director of Masters Orthopedic Program (Geriatric Trauma) at Regions and Methodist Hospitals and the Director of the Mobile Outreach Program. In other words, she is highly accomplished in this area of study.
Dr. Switzer explains why the Masters Orthopedic Program is so vital, “After breaking (fracturing) a hip, the mortality rate is 25% for older adults. There is also a significant risk for losing independence after a hip fracture. The Masters Orthopedic Program is meant to better serve these people who enter the hospitals for orthopedic treatment.”
The Masters Orthopedic Program focuses on three important goals:
- Providing the best, evidence-based, patient-focused, in-hospital care of older patients who have sustained a fracture (broken hip or wrist or spine/back, for example).
- Preventing another fracture from occurring once an initial fracture has been recognized and well treated. A Bone Health Clinic, overseen by Dr. Switzer, functions as an important service where patients gain understanding of osteoporosis, learn strategies to strengthen bones, and are treated, when indicated, for osteoporosis.
- Providing geriatric orthopedic care, including post-op visits, arthritis evaluation and management, and on-site fracture care to older patients who reside in nursing care facilities, such as nursing homes or memory care units. This service, known as Mobile Outreach is the only program in the country in which frail orthopedic patients may be cared for in their residences, as opposed to in the orthopedic clinic.
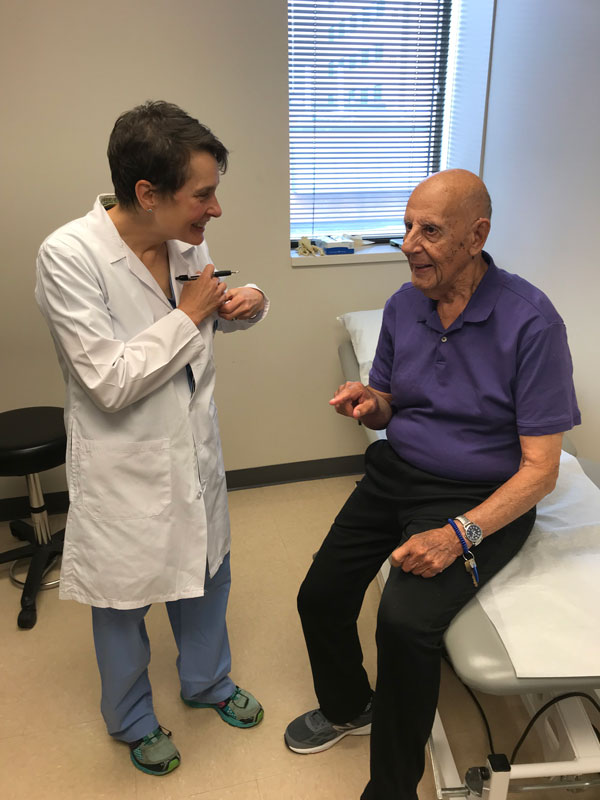
Serving a need that was previously missing, Mobile Outreach is specifically designed for older patients who have a difficult time getting to their post surgery appointments. The program also provides on-site, nonoperative fracture care and care for older individuals with chronic musculoskeletal conditions. “We predominantly go to transitional care facilities, long term care, assisted living, independent living and occasionally to independent homes in special circumstances (ie hospice or frailty situations),” Abell adds.
What can we do to preserve our bone health? Dr. Switzer recommends getting plenty of calcium and vitamin D through foods such as dairy products, leafy greens and fish including salmon and tuna. Incorporate exercise into your daily routine, especially weight bearing (on your feet) activities like walking, running or dancing.
As we and our family members age, it’s comforting we live within a medical community that continually strives to enhance our quality of care.

Elizabeth Abell, Medina resident, nurse practitioner and mobile outreach program coordinator for the western metro shares with LocalTies readers her career trajectory in this exciting venture and how it impacts her daily life.
What is your career background? What is your current title?
I was at Hennepin County Medical Center as a critical care and medical intensive care nurse for five years, five years as a geriatric nurse practitioner for Health Partners primary care, five years at Park Nicollet where I started the orthopedic inpatient management Advanced Practice Clinician team at Methodist Hospital, and now am initiating the mobile outreach program for Park Nicollet orthopedics for the west metro as well as assisting ortho trauma in the operating room at Methodist Hospital two days a week. There was some overlap with the jobs during the transitions.
All of my nursing education was at the University of Minnesota — there I received my bachelor’s in nursing, masters of science as a nurse practitioner and a doctorate in nursing practice.
When did Dr. Switzer approach you for the Mobile Outreach program?
Prior to my starting at Methodist Hospital five years ago, there was a similar position with HealthPartners opening up in the east metro which I considered, but the commute was too far. At the time I said if mobile outreach ever reached the west metro, I’d be extremely interested. Five years later Park Nicollet announced the west metro mobile outreach position at a quarterly meeting – I couldn’t pass on the opportunity. It was difficult to leave the Methodist inpatient position as I LOVED it and everyone I worked with – super bittersweet. The inpatient advanced practice team, since I started, has grown from one (me) to a solid team of three! They are great so there was no better time for me to transition to mobile outreach.
Has this new role changed your day to day routine?
I honestly can say every day, even every hour changes what I thought “my plan” was going to be. I can be out seeing a patient for an hour, get back to my computer, then learn someone with a new fracture needs to be seen the following day that I wasn’t anticipating. I like the variety so far… it’s keeping me on my toes.
How do people qualify to receive treatment?
People who receive the mobile outreach treatment are post operative patients with difficulties with transportation/mobility (especially older adults); new acute fracture patients that are non operative and would like treatment based out of their home (ie: casting, splinting, etc); and those who need management of chronic orthopedic issues (ie: osteoarthritis in older adults requiring steroid I injections). It is basically a “clinic” visit but the provider of care comes to the patient. The main clientele are in long term care, assisted living, independent living, transitional (rehab) care, and some independent homes.
Has this changed your hours worked and your daily schedule?
Most definitely, it is less structured now so I am able to flex my day. I am trying to figure out how best to optimize my time and organize visits as it can be difficult figuring out where I should be going each day. I don’t want to be Elk River and Bloomington the same day — that would be too inefficient. However, as I am ramping up my practice, I am trekking around quite a distance each day. Eventually I will be grouping my visits to regions of the west metro/day.